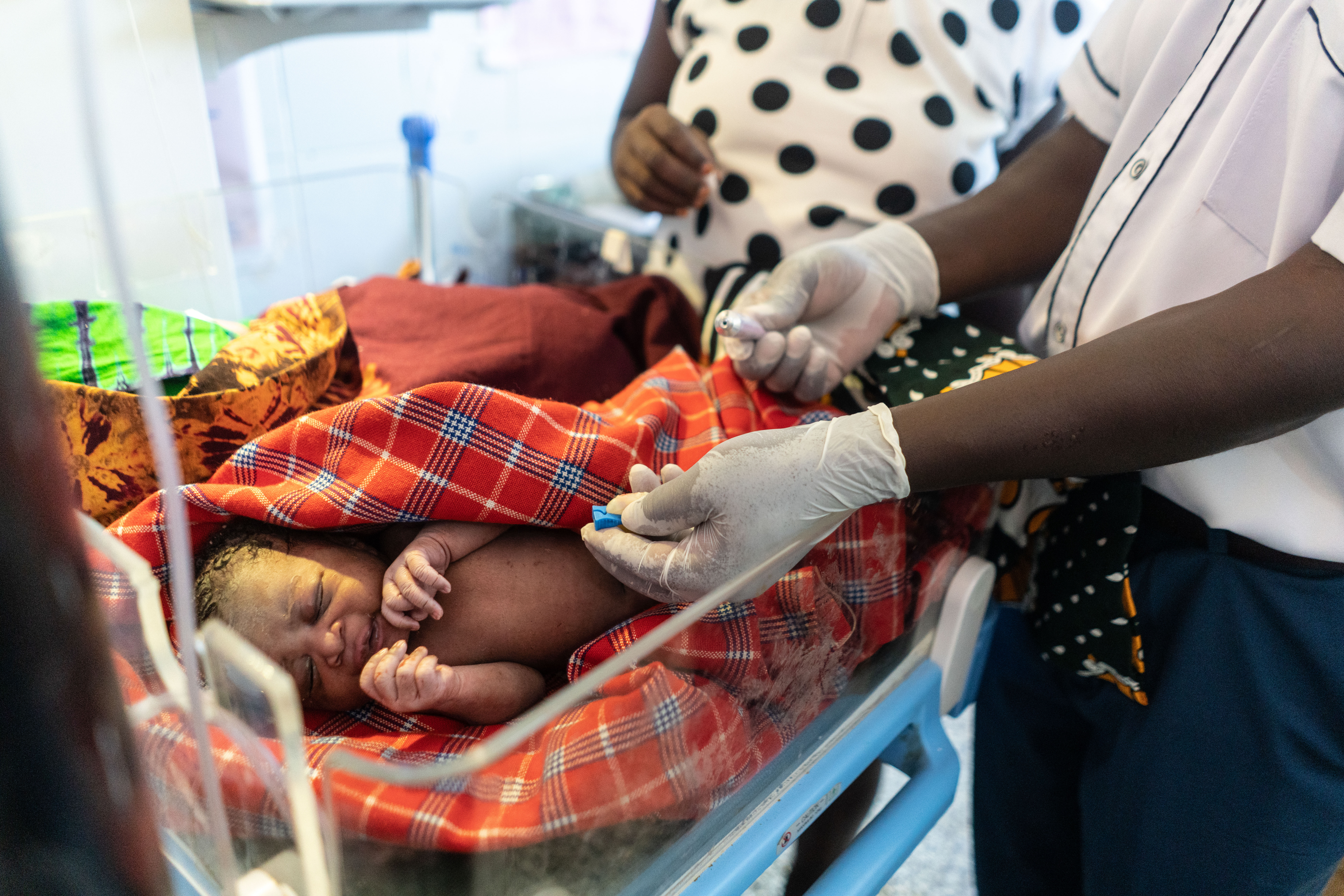
“I want my small sister to grow big and become a police officer,” says Bethwel, who just became a big brother to baby sister Alma.
Alma is just four days old and was born prematurely in a Save the Children and GSK supported hospital in Bungoma, Kenya.
Their mother Maureen explains, “I was shocked because she was not like my first-born child. He weighed 3 kilograms at birth and was chubby. I gave birth to this one who was so small that I hardly had a place to hold. I was terrified.”
At the hospital, Maureen practiced Kangaroo Mother Care (KMC) with baby Alma. KMC is a skin-to-skin connection between mother and baby, where the baby is held to the mother's chest using a sling for many hours. This helped Alma with feeding and bonding with her mum.
Now Maureen has been able to go home and introduce baby Alma to her big brother Bethwel.
“When she is grown, she will pursue her education to a high level. I will show her love,” says Maureen.
“I feel good that my mother has come home with a baby,” Bethwel says. He not only hopes his little sister will be a police officer, but he hopes to join her too - “When I grow up, I will also become a police officer!”